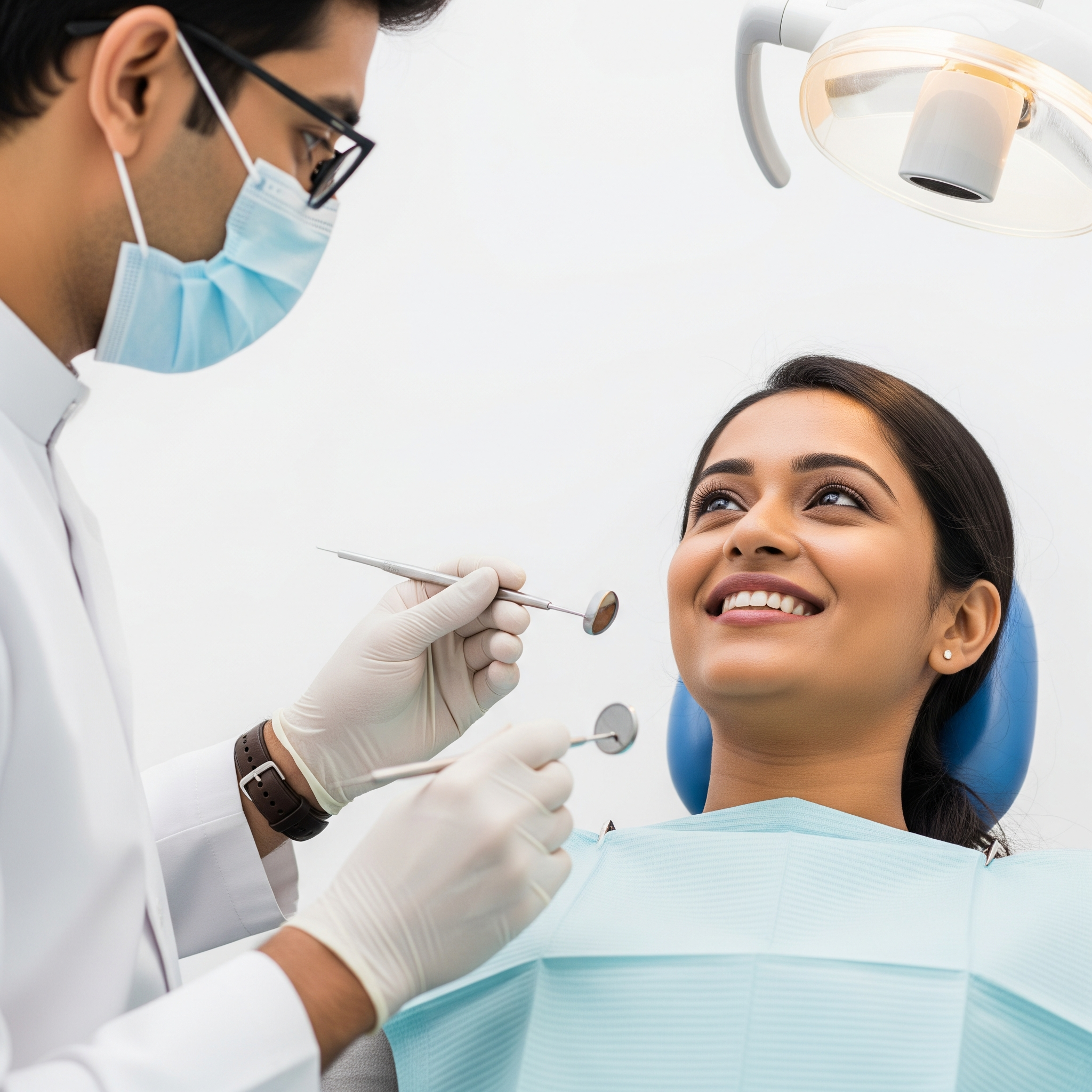
Stain and Calculus

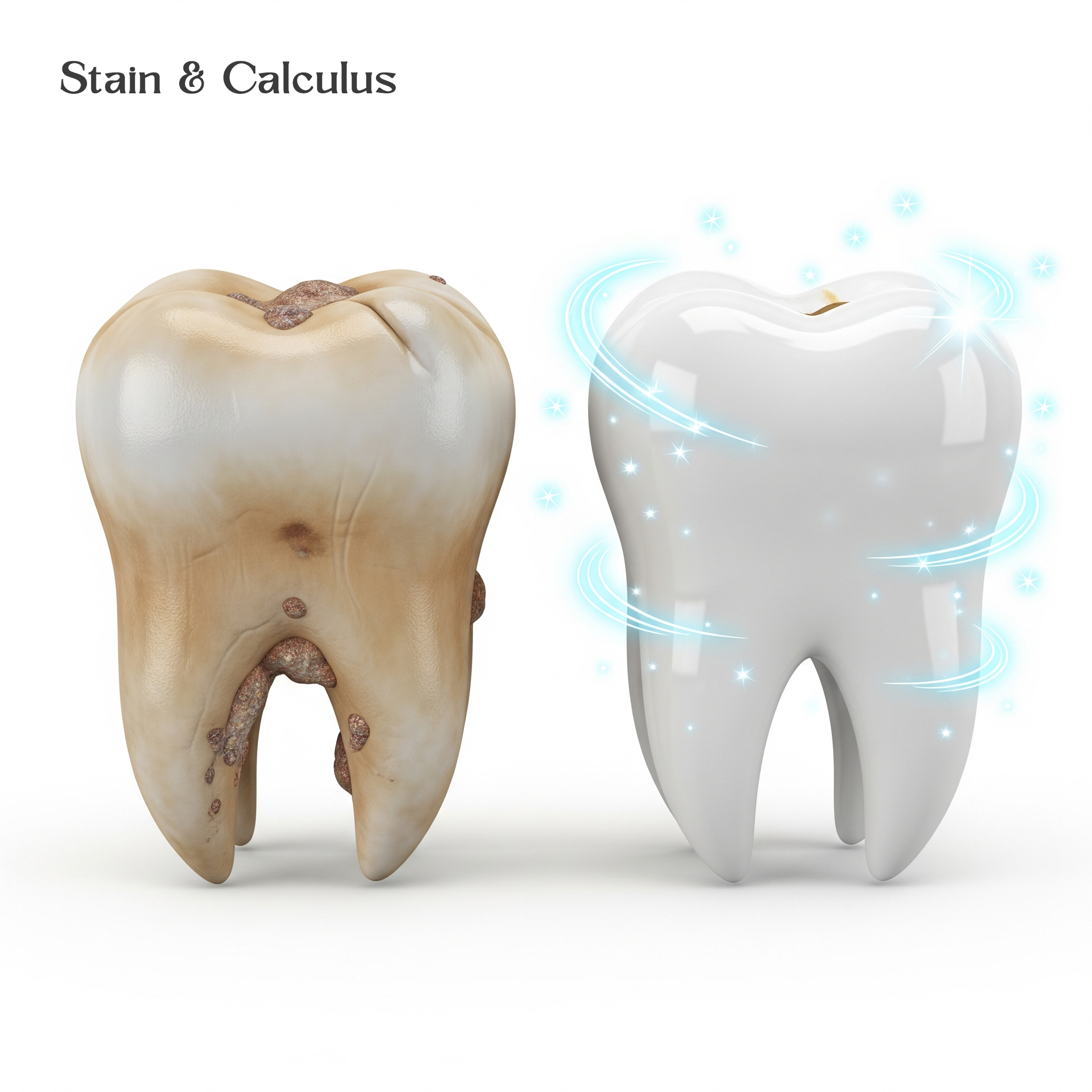
Stain and Calculus: Clear Guide for Patients
Dental stains and calculus are two common conditions that affect the appearance of teeth and the overall health of the mouth. Stains change the color of the teeth, making them appear yellow, brown, black, or even gray. Calculus, also known as tartar, forms when plaque hardens on the teeth and becomes solid. Both issues can lead to gum irritation, bad breath, and long-term dental problems if not treated promptly.
Stains develop either on the outside surface of the tooth or inside the tooth structure. Some stains are easy to remove with professional cleaning, while others need cosmetic treatment. Calculus forms near the gumline and cannot be removed at home with brushing or flossing. Early dental visits help identify these problems before they become difficult to treat.
A clean and healthy mouth reduces the chances of gum disease, cavities, and discoloration. Regular professional cleaning and good home care habits play a major role in preventing stains and calculus. Understanding the types, causes, treatments, and prevention methods helps you maintain a bright and healthy smile.
Types of Stains (Extrinsic vs Intrinsic)
Extrinsic stains sit on the outside of teeth and are usually caused by foods, drinks, tobacco, or poor oral hygiene. These stains are often yellow, brown, or dark and frequently respond well to professional cleaning and polishing. Intrinsic stains are inside the tooth structure (enamel or dentin) and are harder to remove; they can come from trauma, certain medications in childhood, or excessive fluoride.

Intrinsic and extrinsic stains sometimes overlap, and a dentist will evaluate which component dominates. Knowing the type of stain helps the dentist choose the right treatment that restores color and protects tooth structure. Regular photos or shade checks during treatment help monitor progress.
Calculus (Tartar) — What it is and why it matters?
Calculus is mineralized plaque that forms when soft plaque combines with salivary minerals and hardens on teeth. It appears as a hard, yellowish, or brown deposit near the gumline and cannot be removed by brushing or flossing alone. Supragingival calculus forms above the gum and is often chalky; subgingival calculus forms below the gum and tends to be darker and linked to gum infection. If left, calculus causes inflammation, bad breath, gum disease, and even bone or tooth loss over time.
Formation Sites and Clinical Impact
Calculus commonly accumulates on the outer surfaces of upper molars and inner lower front teeth, where saliva pools. Subgingival calculus is hidden beneath the gum margin and promotes pocket formation and chronic inflammation. Both types trap bacteria and increase the chance of gingivitis and periodontitis if not professionally removed. Timely scaling prevents deeper tissue damage and supports long-term oral health.
Quick Signs Patients Notice
Common signs of calculus and stains include a rough feeling on the tooth surface, persistent bad breath, visible discoloration near the gumline, and bleeding gums during brushing. Patients may first notice stains on front teeth or dark bands at the gumline where calculus collects. If you feel a persistent rough or gritty area with your tongue, that could be hardened tartar. Any of these signs warrants a dental check and cleaning.
Treatment — Extrinsic Stains
Extrinsic stains usually respond well to professional dental cleaning, called scaling and polishing, which removes surface deposits and restores brightness. For deeper surface discoloration that resists cleaning, in-office whitening (bleaching) or take-home bleaching trays may be recommended. Lifestyle changes like reducing coffee, tea, cola, and stopping tobacco can prevent recurrence of extrinsic staining.
- Professional scaling & polishing (removes extrinsic stain and soft deposits).
- In-office or at-home bleaching for resistant surface stains.
- Behavioral changes: reduce staining foods/drinks and tobacco use.
After removing extrinsic stains, dentists schedule maintenance cleanings and advise proper home care to slow the return of staining. Frequent polishing may be combined with topical fluoride to protect against enamel sensitivity after whitening. Documenting shade change before and after treatment helps patient satisfaction.
Treatment — Intrinsic Stains
Intrinsic stains require deeper approaches because the pigment is inside the tooth structure and not removable by cleaning. Professional bleaching can lighten some intrinsic stains, but many cases need restorative options such as veneers, bonding, or crowns to mask the discoloration. If intrinsic discoloration arises from a non-vital tooth after trauma, root canal treatment followed by a crown or internal bleaching may be necessary.
Dentists assess the cause of intrinsic staining before choosing treatment; age, tooth health, and patient expectations guide decisions. Conservative options (bleaching) are attempted first when appropriate to preserve natural tooth tissue. Restorative solutions are selected when bleaching is insufficient or when structural damage exists.
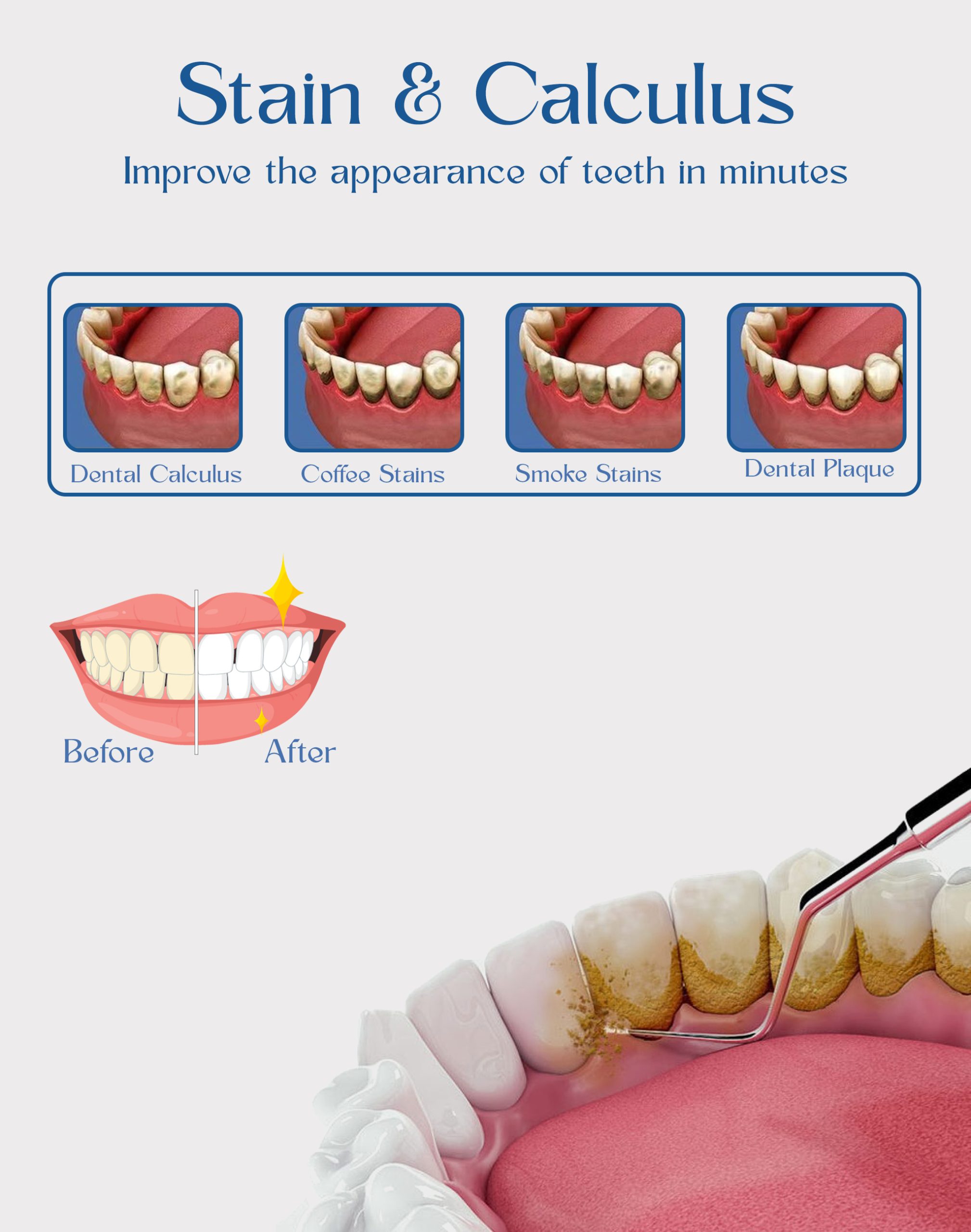
Treatment — Calculus (Scaling & Root Planing)
Once calculus forms, only professional instruments can remove it; this procedure is called scaling and root planing or prophylaxis, depending on severity. Supragingival deposits are removed with hand scalers or ultrasonic devices, while subgingival calculus may need deeper root planing under local anesthesia. After scaling, polishing smooths the tooth surface so plaque is less likely to reattach quickly.
Post-scaling, dentists may recommend more frequent cleanings, improved home care, and adjuncts like chlorhexidine mouthwash for short periods if infection is present. In advanced cases with deep pockets, periodontal therapy or referral to a periodontist may be required to halt disease progression. Regular recall visits are essential to maintain results.
Prevention and Daily Oral Care
Prevention focuses on daily plaque control and regular dental visits every six months or as advised by your dentist. Brush twice daily with correct technique, floss once daily, and limit frequent intake of staining beverages and tobacco to reduce both stains and calculus buildup. Using a tongue scraper and drinking water after meals can lower staining residues and salivary mineral concentration at tooth surfaces.
Professional fluoride, topical polishing during routine visits, and patient education on diet and habits further reduce risk. For patients prone to heavy calculus, more frequent cleanings (3–4 months) may be recommended to prevent recurrence. Early action keeps treatment simple and less costly.
Post-treatment Care and When to See a Dentist
After whitening, scaling, or restorative procedures, follow your dentist’s care instructions to minimize sensitivity or infection risk. Avoid hot drinks, spicy foods, and smoking for 24–48 hours after many procedures; use recommended desensitizing toothpaste if sensitivity occurs. Contact your dentist if you notice persistent pain, swelling, prolonged bleeding after cleaning, or if discoloration returns quickly despite care.
It’s important to maintain good oral hygiene at home by brushing gently, flossing carefully, and using any prescribed mouthwash. Avoid chewing hard or sticky foods on treated teeth to prevent damage to restorations. Drinking plenty of water helps wash away food particles and supports healing. Keeping a balanced diet with minimal sugary foods also aids in long-term dental health.
Seek immediate care for severe gum bleeding, pus discharge, fever, or if a restored tooth feels loose or painful. Early follow-up prevents complications such as dry socket after extractions or recurrent infection under restorations. Keep routine recall visits to maintain both aesthetics and periodontal health. Regular dental check-ups also allow your dentist to monitor any early signs of decay or gum disease and address them promptly.